Running Knee Problems
SPORTS INJURIES
See Also:
![]()
Introduction
Epidemiologic studies indicate that running reduces the threat of some chronic diseases, decreases disability and pain, and lowers healthcare costs. Unfortunately, these benefits can be offset by annual overuse injuries that cause as many as 65% of all runners to stop running and to seek treatment. Running can be viewed as a series of collisions with the ground and the knee is the most common injury site.

The Effects of Running on Menisci and Articular Cartilage
Running is currently one of the most popular sports activities. Nevertheless, the question often arises as to whether the high levels of joint loading involved in running have negative effects. Investigations have shown that forces of up to 300% body weight can occur even during normal walking, and this may rise to 550% during running. Researchers have reported impact forces during running as much as 4 to 8 times higher than those during walking. Articular cartilage contributes to transferring enormous loads as uniformly as possible from one skeletal segment to the next. Whether it manages this task when subjected to the high repetitive loading cycles occurring during long-distance running and can remain intact is still the topic of controversy. Markus Kessler and colaborators investigated the changes in cartilaginous volumes of the tibia, patella, and medial and lateral menisci after extreme dynamic loading as occurs in long-distance runners. Overall, there were significant reductions in volume (P < .05) for the patella, tibia, and menisci. There was evidence of significant change after a running distance of 5 km. A further statistical reduction of the volume could only be demonstrated for the medial meniscus after 10 and 20 km. Tibial, patellar, and meniscal cartilaginous volumes show not only load-dependent volume changes but also an asymptotic curve. This is the first time that meniscal volume changes due to loading have been used as an indicator of the important mechanical contribution that the menisci make to sustaining the knee during repetitive loading. Conclusion: On the basis of the results of this study, the authors assume that the cartilage is able to adapt well to the loads caused by running (1).
The following study was undertaken to examine the rate of recovery from alterations occurring at the knee joint in marathon runners due to loading. After the 20-km run, there was a significant transient decrease in cartilage volume. After 1 hour of rest, no significant reduction of cartilage volume was measured for the patella (–2.1%), the tibia (–1.2%), the lateral meniscus (–3.2%), or the medial meniscus (–5.9%). However, the values recorded for the menisci were borderline, which indicates that recovery of meniscus volume lags behind that of articular cartilage. The data presented in this study indicate a clear tendency toward rapid recovery of the cartilaginous and meniscal volumes at the knee and the results of this study lead to the assumption that the cartilage and the menisci are well able to adapt to the loads caused by running. Conclusion: The articular structures were found to recover rapidly so that exercise could be continued after a short time without reservation (2).
Source:
- Kessler MA, et al.: Volume Changes in the Menisci and Articular Cartilage of Runners An In Vivo Investigation Based on 3-D Magnetic Resonance Imaging. Am J Sports Med May 2006 34:832-836.
- Kessler MA, et al.: Recovery of the Menisci and Articular Cartilage of Runners After Cessation of Exercise Additional Aspects of In Vivo Investigation Based on 3-Dimensional Magnetic Resonance Imaging. Am J Sports Med May 2008 36:966-970.
Running Knee Injuries
Distance running is a significant part of the basic fitness program of many people. However, "serious" distance runners (defined as those who run more than 25 miles per week) face an injury rate of approximately 30% each year. Approximately one third of serious runners will incur an injury in a given year, and approximately one third of the injuries will involve the knee. Biomechanical studies on running reveal the tremendous cyclic forces to which the knee is subjected. The patellar tendon force is around 4.7 to 6.9 times body weight, and patellofemoral joint compressive forces 7.0 to 11.1 times body weight in a jogger. There are several etiologic factors involved, including training errors, anatomic and biomechanical variations, and differences in shoes and running surfaces. Training errors, particularly rapid transitions in training, are responsible for two thirds of injuries. Anterior knee pain is the most common knee complaint, followed by ITBS, ELPS, patellar tendinosis, bursitis, popliteal tenosynovitis, stress fractures, etc. Most knee injuries in runners can be resolved with the use of conservative methods. The most effective biomechanical strategies to reduce load and stress on a locomotor system involve the following factors:
- the movement, such as a change in running style
- the surface (i.e., soft versus hard)
- the shoe (current shoe designs provide variability in cushion effect and motion control of the foot)
- the frequency of repetitive movements (e.g., the mileage, pace, or duration of running).
Source:
- Stan L James, MD: Running Injuries to the Knee. J Am Acad Orthop Surg 1995;3:309-318.
Iliotibial Band Syndrome (ITBS)
Iliotibial band syndrome (ITBS) is the most common cause of lateral knee pain in runners, with an incidence as high as 12% of all running-related overuse injuries. ITBS is believed to result from recurrent friction of the iliotibial band (ITB) sliding over the lateral femoral epicondyle. The ITB is a dense fibrous band of tissue that originates from the anterior superior iliac spine region and extends down the lateral portion of the thigh to the knee. The ITB has insertions on the lateral tibial condyle (the Gerdy tubercle) and the distal portion of the femur. When the knee is extended, the ITB is anterior to the lateral femoral condyle. When the knee is flexed more than 30°, the ITB is posterior to the lateral femoral condyle. Runners with iliotibial band syndrome often demonstrate tenderness on palpation of the lateral femoral condyle approximately 2 cm above the joint line. Tenderness is frequently worse when the patient is in a standing position and the knee is flexed to 30 degrees. At this angle, the iliotibial band slides over the femoral condyle and is at maximal stress, thus reproducing the patient's symptoms Clinically, increased or noticeable tightness of the ITB also may be noted upon examination and performing the Ober's test (the patient lies down on the unaffected side down with the unaffected hip and knee at a 90-degree angle. If the iliotibial band is tight, the patient will have difficulty adducting the affected leg beyond the midline and may experience pain at the lateral knee). A modified Thomas test (which is also called the rectus femoris contraction test or Kendall test) can be performed to assess flexibility of the hip flexors, hamstrings, and the ITB. This test is commonly used to assess rectus femoris muscle flexibility about the knee joint, but the reliability of this test is questioned by several researchers (5).
In patients with iliotibial band syndrome, MRI is very useful diagnostically and shows a thickened iliotibial band over the lateral femoral epicondyle. MRI often detects a fluid collection deep to the iliotibial band in the same region (iliotibial bursa).
This overuse injury occurs with repetitive flexion and extension of the knee. Inflammation and irritation of the iliotibial band also may occur because of a lack of flexibility of the ITB, which can result in an increase in tension on the ITB during the stance phase of running. Other causes or factors that are believed to predispose an athlete to ITBS include excessive internal tibial rotation, genu varum, and increased pronation of the foot.
The main symptom of ITBS is sharp pain or burning on the lateral aspect of the knee. Runners often note that they start out running pain free but develop symptoms after a reproducible time or distance. Early on, symptoms subside shortly after a run, but return with the next run. If ITBS progresses, pain can persist even during walking, particularly when the patient ascends or descends stairs.
Low mileage, recreational runners usually improve with a simple regimen of anti-inflammatory medication and appropriate stretches. However, higher mileage, competitive runners typically require a more comprehensive treatment approach. Treating the condition can be a challenge because underlying myofascial restrictions can significantly contribute to the patient's pain and disability. After acute symptoms are alleviated with activity restriction and modalities, problematic trigger points can be managed with massage therapy or other treatments. A stepwise stretching and strengthening program can expedite patients' return to running. The keys to success for the more resistant cases are myofascial therapy after acute inflammation has been addressed and progression to weight-bearing strengthening exercises, with particular attention to the gluteus medius muscle, before return to running. Corticosteroid injections should be considered if visible swelling or pain with ambulation persists for more than three days after initiating treatment. A small number of patients will not respond to conservative treatment and may require surgical release of the iliotibial band.
Further information:
- John M Martinez, et al. Iliotibial Band Syndrome. eMedicine, December 6, 2006.
- Stephen M Pribut: Iliotibial Band Syndrome. Dr Stephen M Pribut's Sports Pages.
- Owen Anderson and Walt Reynolds: Common knee injuries and runners knee. Sports Injury Bulletin.
- Razib Khaund and Sharon H Flyyn: Iliotibial Band Syndrome: A Common Source of Knee Pain (pdf download). Am Fam Physician, 15 April 2005;71:1545-50.
- Jason D. Peeler and Judy E. Anderson: Reliability limits of the modified Thomas test for assessing rectus femoris muscle flexibility about the knee joint. Journal of Athletic Training, Sept-Oct, 2008.
- M Fredericson, M Guillet, L DeBenedictis. Quick Solutions for Iliotibial Band Syndrome. The Physician and Sportsmedicine, February 2000. Please note that free access to this article is no longer available.
Patellofemoral Pain Syndrome (PFPS) or "Runner's Knee"
We are still working on this section ...
Further information:
- Stephen M Pribut: Runner's Knee (Patellofemoral Pain Syndrome). Dr Stephen M Pribut's Sports Pages.
Patella and Quadriceps Tendinosis
Tendinosis vs. Tendinitis: the term tendinosis was first used in the 1940’s by a group of German researchers, however the term did not receive much attention until it was used again in the mid 1980’s to describe a non-inflammatory tendon condition. The more commonly used term of tendinitis has since been proven to be a misnomer for several reasons. The first of which is that there is a lack of inflammation in conditions that were typically called a tendonitis. Since inflammation is the key pathological process involved with that term, and the discovery that there in fact were no, or very few, inflammatory cells present in the condition, a new term tendinosis was adopted. This has a profound impact on how the condition is treated.
Treatment Options: although the surgical treatment of patellar tendinopathy is a common procedure, there have been no randomized, controlled trials comparing this treatment with forms of non-operative treatment. The purpose of the study conducted by Roald Bahr and colaborators was to compare the outcome of open patellar tenotomy with that of eccentric strength training in patients with patellar tendinopathy. Although surgical treatment and eccentric strength training can produce significant improvement in terms of pain and function scores, it appears that only about half of all patients will be able to return to sport within one year after treatment with each option, and fewer still will have relief of all symptoms. In the absence of other validated treatment options, authors believe that eccentric training, a low-risk and low-cost option, should be tried before surgery is considered. Conslusion: No advantage was demonstrated for surgical treatment compared with eccentric strength training. Eccentric training should be tried for twelve weeks before open tenotomy is considered for the treatment of patellar tendinopathy (2).
Eccentric exercises: "the key to the rationale behind eccentric drills is that they are the best way of promoting tendon remodelling - the regrowth and reordering of fibrous tissue in place of the denser, degenerative tissue typical of tendinosis. The athlete needs to be taught eccentric exercises (see table below). A 45-degree slope is required and (at a later stage) a weights bar. Initially the athlete stands straight on the slope, then flexes his/her knees to 90 degrees, returning to a straight position again. The movement down must be done slowly (to a count of three) and the return can be done quickly (to a count of one). When away from home the slope can be replaced by the edge of a curb or step so that opportunities can be taken whenever possible to do the drills. The number of repetitions is determined by the amount of discomfort felt in the patellar tendon. I advise athletes to stop a sequence of repetitions when they perceive an ache in the patellar tendon of 3/10, using the scale described above. The rationale for this is to stimulate the patellar tendon eccentrically to a fixed (symptomatic) level each day, but without such a high score as to produce pain and further damage. I suggest to athletes that they can do these repetitions as often as possible every day and many achieve the repetitions 3 to 4 times a day. The exercise sequence can be progressed as shown in Table 1. For some athletes stage 1 is too easy and they cannot bring on any discomfort in the patellar tendon. For others, the rate-limiting factor is quadriceps fatigue and for this reason they can use two legs in returning to the standing position (see stages 2 to 4).
Stage |
Exercise |
1 |
Two legs, 90 degree squat, no slope |
2 |
Two legs, 90 degree squat on 45 degree slope |
3 |
Single leg for squat phase (eccentric); two legs return phase (concentric), on slope |
4 |
10kg bar; single leg for squat phase, two legs return, on slope |
5 |
Single leg only throughout, on slope |
As the stages progress the athlete will be able to increase the number of repetitions they can perform before the symptoms come on at a discomfort level of 3/10. There will be some days when the athlete can manage more repetitions than others, but normally they will be able to move on to the next stage after 2 to 4 weeks -- so improvement in this condition is usually measured in months, not weeks. The rate of progression will vary from athlete to athlete, dependent in large part on how often they perform the exercises. If more pain occurs in the tendon, the athlete should be advised to rest for 2 to 3 days and then drop back one stage in the rehab exercise progression."
- Source (text on eccentric exercises and the table) and more information: Patellar tendinitis: why patellar tendinitis is usually the wrong diagnosis for patellar tendon pain, and how to banish patellar tendon pain? Sports Injury Bulletin.
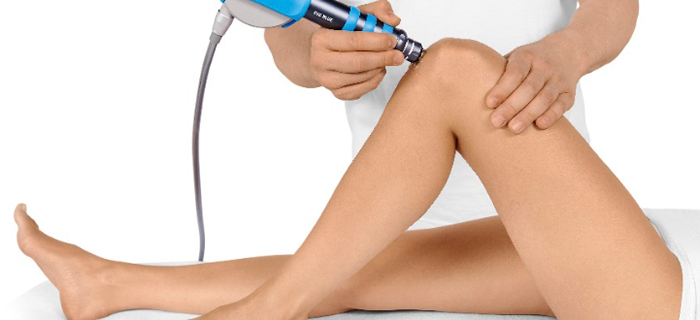
Shockwave Treatment: Extracorporeal Shock Wave Therapy (ESWT) is the application of Shock Waves in medicine. It is clinically proven that pressure waves, when applied to injured tissues, stimulate metabolic reactions: reduction of pain felt by nerve fibers, increase of blood circulation in surrounding soft tissues, beginning of healing process triggered by stem cells activation. Patients not responding to conservative treatment for six months should undergo radial shock wave therapy (RSWT), which usually requires three weekly sessions. Shockwave Therapy can be used to treat longstanding pain and discomfort. We use an EMS Swiss DolorClast shockwave machine. A hand-held device is moved over a conductive gel on the skin to send waves of energy to patella or quadriceps tendons. These mechanical pressure pulses – known as shockwaves - work by reinjuring tendons and surrounding tissues, which in turn stimulates blood flow helping problem areas to heal (neoangiogenesis). The results are not instant, the treatment may be uncomfortable and the results can be operator dependent. A Shockwave applied to a problem area, but without correcting the underlying adverse biomechanics will not work. Correcting causative factors in combination with Shockwave treatment create the best outcomes and the holistic, whole body approach, means you have much better chance of recovery. Addressing the immediate symptoms is an important step to recovery and can help uncover potential underlying issues that need to be resolved. Shockwave is a major advance in effective, safe non-surgical treatment.
Further information:
- Andrea Ferretti, et al.: Patellar Tendinosis. A Follow-up Study of Surgical Treatment. The Journal of Bone and Joint Surgery (American) 84:2179-2185 (2002).
- Roald Bahr, et al.: Surgical Treatment Compared with Eccentric Training for Patellar Tendinopathy. A Randomized, Controlled Trial. The Journal of Bone and Joint Surgery (American). 2006;88:1689-1698.
- Paul Morrissey: The Shockwave Solution. 2016
Other Running Injuries
We do knees only and therefore this page focuses on running knee injuries. However, you can find detailed information on other running problems here:
- Piriformis Syndrome
- Iliopsoas Tendonitis
- Shin Splints or Medial Tibial Stress Syndrome (MTSS)
- Achilles Tendinopathy
- Plantar Fasciitis
Selecting Running Shoes
There is no single best running shoe as everyone has different needs. Your biomechanics and gait patterns, the size and the shape of your feet, your weight and the surfaces you run on all play an important role in selecting the best possible running shoes. There are several factors that you need to take into consideration to make sure that you make the right choice:
- What is the shape of your feet (normal, flat, high-arched)?
- Do you overpronate, underpronate or have a neutral landing?
- Will you use shoes for trail running, competition, or just general fitness?
- Do you have a history of injury, do you need extra cushioning?
- Past experience with different shoes and problems with current shoes
In addition to foot type and leg malalignment, research has identified type and wear of running shoes as risk factors for the development of overuse injuries. Proper shoe selection and fit can compensate for biomechanical abnormalities and decrease injury rates.
Specialists can use the basics of foot types, gait patterns, and running shoe design to perform a simple biomechanical assessment to help you with selecting the best possible running shoes. They can help you not only with fit but also review desired shoe characteristics with you. One of the best means of finding out information about running shoes is to locate a good running shoe store, that maintains an excellent reputation among your local running community. 
It is likely that you have probably been wearing your old shoe for too long. Failing to replace worn shoes is a major cause of running injuries. Estimates vary, as do individuals, as to when is the best time to replace your running shoes. The usual estimates place the mileage at somewhere between 350 and 550 miles. This means that many individuals should be replacing their shoes before they show major wear. In spite of the lack of wear the shoe will be gradually losing its shock absorption capacity as well as possibly starting to loose some of its stability.
Numerous studies have demonstrated that well-designed and properly fitted running shoes reduce the number of running-related overuse injuries.
Further information:
- Stephen M Pribut: Selecting and Fitting a Running Shoe. Dr Stephen M Pribut's Sports Pages.
- Chad A. Asplund and David L. Brown. The Running Shoe Prescription. The Physician and Sportsmedicine, January 2005. Please note that free access to this article is no longer available.
- Jeff Ray. How to Choose a Running Shoe. TheRunningAdvisor.com
- REI staff. How to Choose Running Shoes. REI Expert Advice.
Stretching
Stretching has been promoted as a method to prevent injury and improve athletic performance. Although research suggests that this may be true for regular stretching performed every day, an isolated act of stretching immediately before exercise likely has no effect on injury prevention and actually impairs performance in strength and power sports. Basically, stretching immediately before exercise will not prevent injuries. It reduces force and power by about 2% to 5%, with conflicting study results about its effect on running speed. Regular stretching over weeks increases force and power by about 2% to 5% and improves 50 yard running speed by about 0.06 second. If the objective is to increase force or power in athletic performance, stretching should not be performed before activity. If the objective is to increase speed, it may or may not be beneficial to stretch immediately before activity (1).

However, Dr Pribut believes that regular stretching may help reduce running injuries: "Runners frequently develop tightness in the posterior muscle groups. This includes the hamstrings and the calf muscles. The quadriceps and anterior shin muscles may become relatively weak, due to muscular imbalance. The abdominal muscles also tend to be weak on runners who do not exercise them. The calf (achilles) should be gently stretched and so should the hamstrings. The best stretch for the calf muscles is the "wall stretch". I recommend stretching one set of leg muscles at a time. One leg is back, knee straight, the other leg is forward with the knee bent. The leg that is back is being stretched. Ten repetitions holding for 10 seconds each is ideal. There are several different stretches to choose from for the hamstrings: Forward bends with the knees slightly bent, knee to chest or leaning forward with the leg out straight in front of you all work. It is important to not aggravate your back while performing hamstring stretches. Stretching early in the morning can be difficult before you have loosened up. It is also hard to stretch before your muscles have warmed up. Be very gentle when stretching prior to a run. If you have had achilles tendonitis or tight calf muscles, that you have for the most part recovered from and are on a maintainance stretching program, you might find it helpful to stretch about 1/2 to 3/4 of a mile into your run. The muscles will have warmed up and be better prepared to be stretched." (2).
- Ian Shrier: When and Whom to Stretch? Gauging the Benefits and Drawbacks for Individual Patients. The Physician and Sportsmedicine, March 2005. Please note that free access to this article is no longer available.
- Stephen M Pribut: When should I start stretching and when is it bad to start? Dr Stephen M Pribut's Sports Pages.
Further information on running knee injuries:
- Stephen P. Messier et al.: Risk Factors and Mechanisms of Knee Injury in Runners. Medscape Orthopaedics, 12 November 2008*. Summary: Although running injuries are well understood medically, their potential risk factors are not. Thus, we presently have limited ability to identify individuals at high risk for overuse injuries. The results of this study relate larger knee joint loads to poor hamstring flexibility, greater body weight, greater weekly mileage, and greater muscular strength. Most of these risk factors could potentially be modified to reduce joint loads to lower the risk of injury. * Please note that you may need to register to be able to read Medscape Orthopaedics articles.
- Gretchen Reynolds: Can Running Actually Help Your Knees? The New York Times online, August 11, 2009.
This page was launched on 21 January 2009 and updated on 26 June 2018.
Site last updated on: 28 March 2014
|
[ back to top ]
 Disclaimer: This website is a source of information
and education resource for health professionals and individuals
with knee problems. Neither Chester Knee Clinic nor Vladimir Bobic
make any warranties or guarantees that the information contained
herein is accurate or complete, and are not responsible for
any errors or omissions therein, or for the results obtained from
the use of such information. Users of this information are encouraged
to confirm the accuracy and applicability thereof with other sources.
Not all knee conditions and treatment modalities are described
on this website. The opinions and methods of diagnosis and treatment
change inevitably and rapidly as new information becomes available,
and therefore the information in this website does not necessarily
represent the most current thoughts or methods. The content of
this website is provided for information only and is not intended
to be used for diagnosis or treatment or as a substitute for consultation
with your own doctor or a specialist. Email
addresses supplied are provided for basic enquiries and should
not be used for urgent or emergency requests, treatment of any
knee injuries or conditions or to transmit confidential or medical
information. If you have sustained a knee injury or have a medical condition,
you should promptly seek appropriate medical advice from your local
doctor. Any opinions or information,
unless otherwise stated, are those of Vladimir Bobic, and in no
way claim to represent the views of any other medical professionals
or institutions, including Nuffield Health and Spire Hospitals. Chester
Knee Clinic will not be liable for any direct, indirect,
consequential, special, exemplary, or other damages, loss or injury
to persons which may occur by the user's reliance on any statements,
information or advice contained in this website. Chester Knee Clinic is
not responsible for the content of external websites.
Disclaimer: This website is a source of information
and education resource for health professionals and individuals
with knee problems. Neither Chester Knee Clinic nor Vladimir Bobic
make any warranties or guarantees that the information contained
herein is accurate or complete, and are not responsible for
any errors or omissions therein, or for the results obtained from
the use of such information. Users of this information are encouraged
to confirm the accuracy and applicability thereof with other sources.
Not all knee conditions and treatment modalities are described
on this website. The opinions and methods of diagnosis and treatment
change inevitably and rapidly as new information becomes available,
and therefore the information in this website does not necessarily
represent the most current thoughts or methods. The content of
this website is provided for information only and is not intended
to be used for diagnosis or treatment or as a substitute for consultation
with your own doctor or a specialist. Email
addresses supplied are provided for basic enquiries and should
not be used for urgent or emergency requests, treatment of any
knee injuries or conditions or to transmit confidential or medical
information. If you have sustained a knee injury or have a medical condition,
you should promptly seek appropriate medical advice from your local
doctor. Any opinions or information,
unless otherwise stated, are those of Vladimir Bobic, and in no
way claim to represent the views of any other medical professionals
or institutions, including Nuffield Health and Spire Hospitals. Chester
Knee Clinic will not be liable for any direct, indirect,
consequential, special, exemplary, or other damages, loss or injury
to persons which may occur by the user's reliance on any statements,
information or advice contained in this website. Chester Knee Clinic is
not responsible for the content of external websites.