Knee Imaging
IMAGING TECHNIQUES
See also:
- MRI Image Gallery (under construction)
- Please visit our Pinterest MR Image board
- Glossary of Knee Terms
Introduction
Over the past 20 years the diagnosis of knee disorders have been improved enormously through better imaging techniques.
Radiography (X-ray)
Radiographs of the knee are usually the first imaging studies, especially if bone wear and tear is suspected clinically. Weight-bearing radiographs are helpful in assessing the extent of arthritis in the knee joint and in planning various joint resurfacing procedures.
 |
|
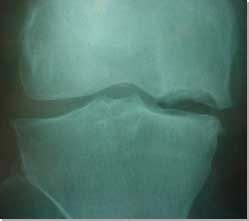
| Osteochondral
defect (OCD) of the medial femoral condyle. |
Radiographs are often required after acute knee trauma. If the trauma is severe, and the injured person complains of severe pain and inability to bear weight, fractures must be ruled out. Anterioposterior and lateral radiographs of the knee best visualise the tibio-femoral and tibio-fibular joints. The skyline, or tangential, view allows the assessment of the patellofemoral joint and provides an unobstructed view of the patella. Stress radiographs (the knee is forced manually into varus or valgus position) can demonstrate ligament deficiency, but this technique is rarely used nowadays.
Further Information
-
RadiologyInfo is designed to answer your questions related to many radiologic procedures and therapies available. This web site provides you with information on how various x-ray, CT, MRI, ultrasound, bone-scan, and other procedures are performed. It also addresses what you may experience and how to prepare for the exams. All material on the RadiologyInfo web site is reviewed and approved by experts in the field of radiology from the ACR and RSNA, as well as other professional radiology organizations.
-
GE Healthcare has decided to publish this famous Textbook of Radiology on the web. It is freely available online to the global community of medical imaging.
-
Paul J. Nugent: Avoiding Unnecessary Radiographs in Sports: The Ottawa Knee Rule. The Physician and Sportsmedicine, May 2004. Please note that free access to this article is no longer available.
Ultrasound
Diagnostic ultrasonography is useful in imaging the soft tissues about the knee, muscle injury, bone healing, and foreign bodies. Recent technologic improvements have made this imaging modality increasingly more accurate while providing significant benefits over traditional modalities such as magnetic resonance imaging, particularly regarding cost, patient satisfaction, and ease of usage. Increasing use of diagnostic ultrasonography for musculoskeletal conditions is likely as acceptance grows.
For example sonographic appearances in jumper's knee reveal a focal hypoechoic area combined with various amounts of swelling of the surrounding tendon. Hyperechoic areas represent tendinosis, not tendinitis, although the two terms are often used interchangeably. Radiologists should emphasize that in adults, clinical correlation with imaging is essential, and especially that the finding of a focal hypoechoic region is not necessarily an indication for surgery. Also, after patellar "decompression" or tenotomy, routine postoperative imaging is not a useful guide to management. The time for patients to recover from surgery is six to 12 months, so clinicians should not expect clinical or radiological recovery before then.
See Also:
-
Jill L Cook, et al. Jumper'’s knee’ images need clinical backup: Ultrasound shows promise for predicting patellar tendinopathy in young athletes. A supplement to the September 2000 issue of Diagnostic Imaging
Magnetic Resonance Imaging (MRI)
MRI is an imaging technique used to get cross-sectional images using strong magnetic field and radio waves (radio frequency pulses) instead of X-rays. In MRI scanning, patients are placed inside a very large and strong magnet, so that all the protons in the atoms of the patient's body can be aligned to a magnetic field. Then, radio waves (called radio frequency pulses) are directed at the protons (the nuclei of hydrogen atoms) to excite the protons.
 |
|
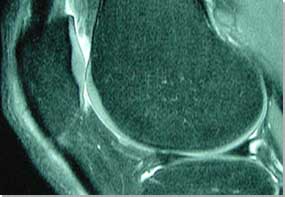
| MR image of the knee - articular
cartilage is shown particularly well. |
Once the radio waves are stopped, excited atoms emit radio signals
received by an antenna (a surface coil in the MRI machine), which are
then measured and processed to form an image using a computer. In the
human body, protons are most abundant in the hydrogen atoms of water.
Thus, MRI images represent the water content in the area of the exam.
The more water present, the more radio signals emitted, and the whiter
the image. All intra-articular structures, including menisci, ligaments
and articulating surfaces, can be visualised in great detail. The indications
for MRI of the knee are difficult to define and depend on the specific
clinical situation and the particular information needed. Routine MR
knee imaging is usually very accurate and helpful diagnostically. MRI is also safe. There are no known side effects to having an MRI
scan performed but you should be aware of the following:
- The strong magnetic field can cause metal implants to dislodge,
burn,and causeadditional injuries. When you have any metal implant
in your body, such as a pacemaker, prosthetic valves, or clips, you
should let your radiologist or MR technician know. If it is not confirmed
to be compatible with the magnet, you should not take the MRI. If
you have had bullet injuries or possible metal fragments in your body,
X-rays can be taken instead for detection of metal objects.
- Metallic implants or fragments that might be affected by magnet:
Cardiac pacemakers, Artificial cardiac valves, Cerebral aneurysm clips,
vascular clips, Epidural electrodes, Prosthetic (implanted) hip, knee
or ankle joint, Chemotherapy or insulin pumps, Intrauterine device
(IUD), Metallic bone plates, pins, screws, surgical staples, especially
within 4-6 weeks after surgery, Bullets, shrapnel, metal fragments,
especially in and around eyes, Metallic ear implants, etc.
- Women in the first 12 weeks of pregnancy should avoid MRI and the
contrast medium. There are no known harmful effects to pregnant women
and unborn babies. However, because it is a recently-developed technology,
the long term effects of MRI are not known.
- Allergic reactions to the contrast medium are possible, but very
rare.
- Claustrophobia: lying alone inside the tunnel of huge magnet may provoke intense fear of confinement. If you hav any history of claustrophobia, you should inform your radiologist or technologist. Sedatives can be given before scanning.
A new MRI Scanner at Nuffield Health, The Grosvenor Hospital Chester
We have a new fixed MRI scanner at the Grosvenor Nuffield Hospital in Chester. The unit is available for MR imaging throughout the week. We have maintained the same quality of knee MR imaging, and sub-specialist expertise with an emphasis on articular cartilage and subchondral imaging. We store all MR images on a dedicated secure server and continue to provide our patients with a CD with a complete set of DICOM images, if requested.
If required, we can offer MR imaging and a knee consultation on the same day, but we need a couple of weeks notice to synchronise both appointments. Please note that consultant radiologist's MRI report may not be available on the same day.
Our web-based Kodak MRI teleradiology system, has been replaced with a PACS system in 2008.
To download a brochure on MR imaging click on: About Your Scan
Further information on MR Imaging:
-
for more info on MR imaging go to: www.radiologyinfo.org/content/mr_musculoskeletal.htm
-
if you are interested in MRI history please read this article: http://www.isbe.man.ac.uk/personal/dellard/dje/history_mri/history%20of%20mri.htm
-
for X-ray and MRI safety issues go to: www.radiologyinfo.org/content/safety/rad_safety.htm
-
for more information on MR imaging of the knee please read this article:
Magnetic resonance imaging of the knee. Eugene G McNally, BMJ 20 July 2002 -
for more information on articular cartilage MR imaging please read this article:
Magnetic resonance imaging of articular cartilage defects and repair. Vladimir Bobic, ISAKOS Current Concepts. - to hear a sound of an MRI scanner click on: Sound of MRI scanner (.wav file).
-
to download Dr David Ritchie's CKC MRI Protocol click on: Chester Knee Clinic MRI Protocols

Arthroscopy
Arthroscopy is a surgical procedure which orthopaedic surgeons use to view, diagnose and treat problems inside the knee joint. For more information on knee arthroscopy please see our separate page Arthroscopic Surgery.
Page last updated on 12 May 2018
Site last updated on: 28 March 2014
|
[ back to top ]
 Disclaimer: This website is a source of information
and education resource for health professionals and individuals
with knee problems. Neither Chester Knee Clinic nor Vladimir Bobic
make any warranties or guarantees that the information contained
herein is accurate or complete, and are not responsible for
any errors or omissions therein, or for the results obtained from
the use of such information. Users of this information are encouraged
to confirm the accuracy and applicability thereof with other sources.
Not all knee conditions and treatment modalities are described
on this website. The opinions and methods of diagnosis and treatment
change inevitably and rapidly as new information becomes available,
and therefore the information in this website does not necessarily
represent the most current thoughts or methods. The content of
this website is provided for information only and is not intended
to be used for diagnosis or treatment or as a substitute for consultation
with your own doctor or a specialist. Email
addresses supplied are provided for basic enquiries and should
not be used for urgent or emergency requests, treatment of any
knee injuries or conditions or to transmit confidential or medical
information. If you have sustained a knee injury or have a medical condition,
you should promptly seek appropriate medical advice from your local
doctor. Any opinions or information,
unless otherwise stated, are those of Vladimir Bobic, and in no
way claim to represent the views of any other medical professionals
or institutions, including Nuffield Health and Spire Hospitals. Chester
Knee Clinic will not be liable for any direct, indirect,
consequential, special, exemplary, or other damages, loss or injury
to persons which may occur by the user's reliance on any statements,
information or advice contained in this website. Chester Knee Clinic is
not responsible for the content of external websites.
Disclaimer: This website is a source of information
and education resource for health professionals and individuals
with knee problems. Neither Chester Knee Clinic nor Vladimir Bobic
make any warranties or guarantees that the information contained
herein is accurate or complete, and are not responsible for
any errors or omissions therein, or for the results obtained from
the use of such information. Users of this information are encouraged
to confirm the accuracy and applicability thereof with other sources.
Not all knee conditions and treatment modalities are described
on this website. The opinions and methods of diagnosis and treatment
change inevitably and rapidly as new information becomes available,
and therefore the information in this website does not necessarily
represent the most current thoughts or methods. The content of
this website is provided for information only and is not intended
to be used for diagnosis or treatment or as a substitute for consultation
with your own doctor or a specialist. Email
addresses supplied are provided for basic enquiries and should
not be used for urgent or emergency requests, treatment of any
knee injuries or conditions or to transmit confidential or medical
information. If you have sustained a knee injury or have a medical condition,
you should promptly seek appropriate medical advice from your local
doctor. Any opinions or information,
unless otherwise stated, are those of Vladimir Bobic, and in no
way claim to represent the views of any other medical professionals
or institutions, including Nuffield Health and Spire Hospitals. Chester
Knee Clinic will not be liable for any direct, indirect,
consequential, special, exemplary, or other damages, loss or injury
to persons which may occur by the user's reliance on any statements,
information or advice contained in this website. Chester Knee Clinic is
not responsible for the content of external websites.